Join us for our next webinar!
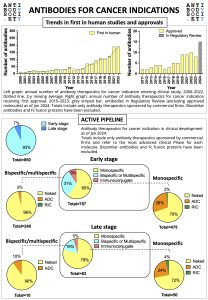
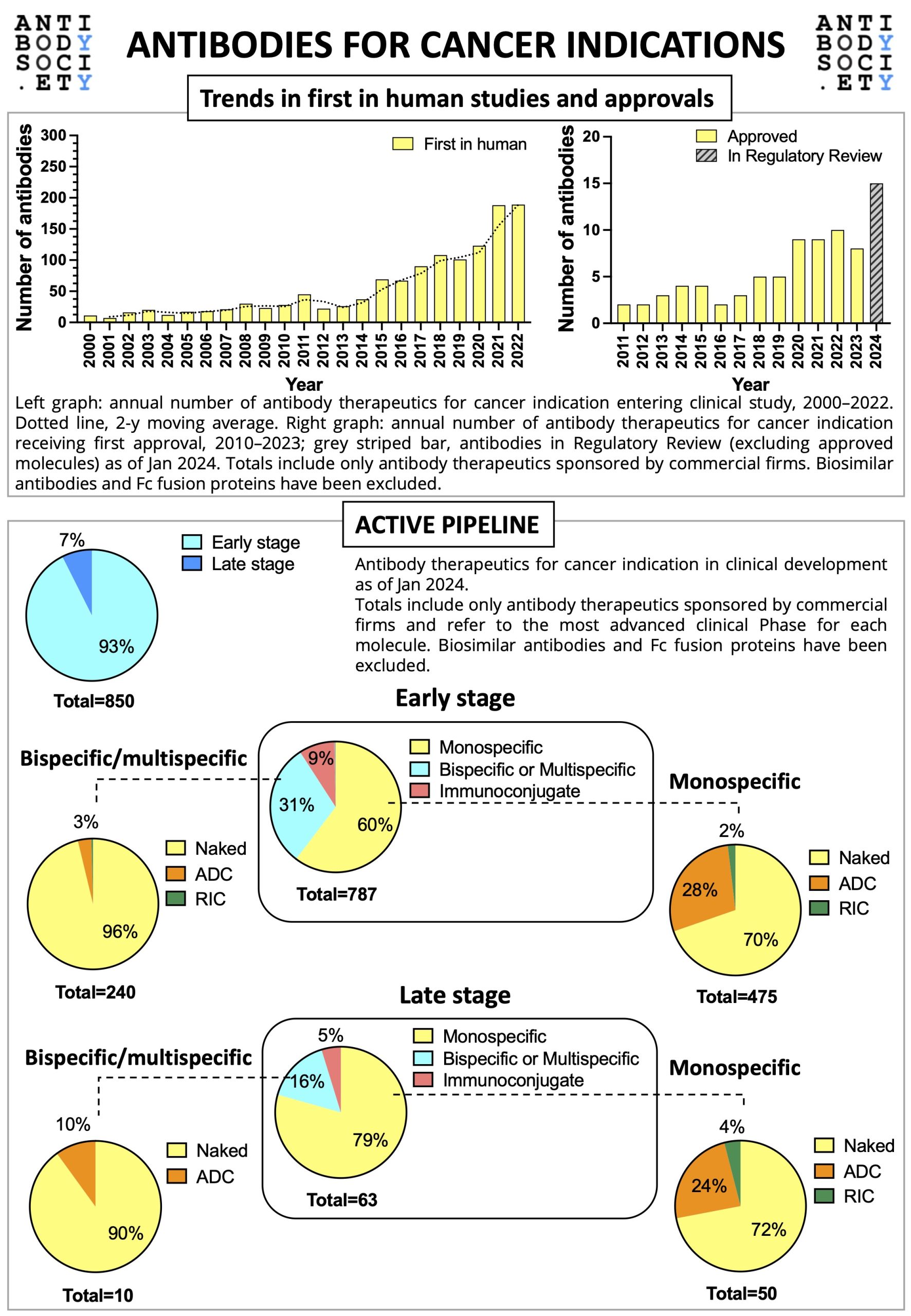
Antibody-drug conjugates (ADCs) have emerged as an important class of targeted therapeutics, combining the targeting specificity of antibodies with the potency of cytotoxic drugs. Recent advances in ADC research have led to improved stability, efficacy, and safety. There is a clear trend within Antibody therapeutics towards ADCs with the improvement of novel technologies to address a growing cancer population worldwide.
However, developing effective ADCs is expensive and poses unique informatics challenges. Researchers must integrate data across multiple modalities – from antibody discovery and engineering to small molecule payload development and optimization. Seamless collaboration between immunologists, protein engineers, chemists, and pharmacologists are essential.
The Signals™ Research Suite is the first integrated informatics platform purpose-built to accelerate multi-modal drug development like ADCs and is composed of a trio of scientific software applications:
- Signals™ Notebook: The premier cloud-based electronic lab notebook that facilitates creation and communication about molecules of interest via hierarchical editing language for macromolecules (HELM), powered Chemdraw®.
- Signals™ VitroVivo: For data analysis, visualization, and curve fitting bioassay results for standardized and consistent results, powered by Spotfire®.
- Signals™ Inventa: Enabling multi-assay or multi-study comparison, powered by Spotfire, with the ability to find the best candidate to move forward, accelerating decision making. Researchers gain better visibility into ADC candidate profiling and can quickly determine structure-activity and structure-property relationships across modalities to select optimal conjugation sites and pairings.
Attendees will gain insights into the latest trends and challenges in ADC development, informed by recent research and advancements in the field. The presentation will also emphasize the importance of integrating various data types and sources in the ADC development process, showcasing how the Signals Research Suite facilitates this integration, thereby driving more efficient, safer drug development.
About the speaker:
Dr. Wisotsky attended the University of California, Santa Cruz with a focus on molecular and cellular biology. He obtained his Ph.D. at the University of California, Riverside for Neuroscience where he worked on taste detection from molecular mechanism to behavioral outcomes in fruit flies. Subsequently Zev joined startup companies with the focus to support scientists getting their science done more efficiently. He has worked within pre-sales teams to discover, consult, and deliver software solutions that meet customer needs both scientifically and technically. Today he is a Revvity Senior Principle Marketing Manager for Biologics in the Signals Suite.
Registration is open!